What is AVRT?
 Sarah Marsh
Sarah Marsh 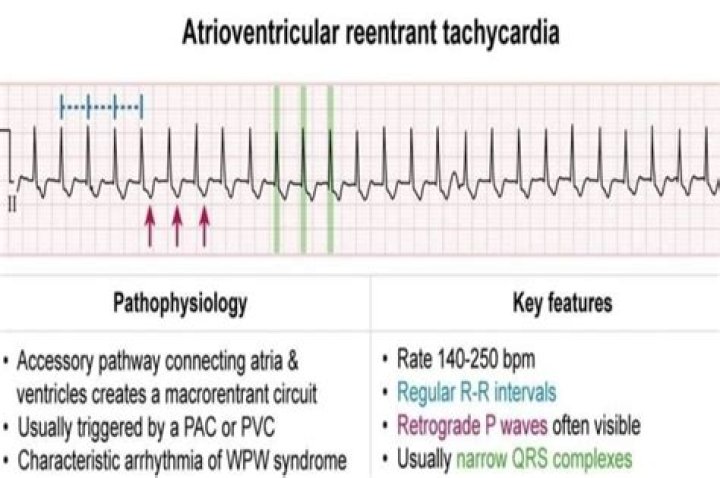
Besides, what causes AVRT?
It results from an extra connection between your upper and lower chambers. You might hear it called atrioventricular reciprocating tachycardia. AVRT is more likely to happen when you're a child or teenager. It doesn't mean you have other heart problems.
Secondly, is AVRT the same as WPW? The difference between this typical AVRT and the AVRT seen with WPW is that, in WPW, the accessory pathway is capable of conducting electrical impulses in both directions — from the atrium to the ventricle as well as from the ventricle to the atrium.
Considering this, what is the difference between AVRT and avnrt?
Pathophysiology. AVNRT and AVRT are electrical aberrancies that occur mainly as a result of reentry. AT can result from one of the three mechanisms (Table 1). 3–6 AVNRT and AVRT are atrioventricular nodal-dependent arrhythmias, whereas AT is an atrioventricular nodal-independent arrhythmia.
What are the 3 types of SVT?
There are three major types of supraventricular tachycardia:
- Atrioventricular nodal reentrant tachycardia (AVNRT).
- Atrioventricular reciprocating tachycardia (AVRT).
- Atrial tachycardia.
Related Question Answers
What does avnrt feel like?
AVNRT is the most common type of supraventricular tachycardia, and it is more common in women than men (approximately 75% of cases occur in females). The main symptom is heart palpitations, which is a sensation that feels like the heart is beating too hard, fluttering, or skipping a beat.What is Orthodromic AVRT?
Orthodromic AVRT means that the ventricles are depolarized normally via the atrioventricular node and His-Purkinje system (Figure 3). Because the impulse reaches the ventricles through the His-Purkinje network the QRS complexes will appear normal (i.e QRS duration will be <0.12 s).What is WPW on ECG?
In Wolff-Parkinson-White (WPW) syndrome, an extra electrical pathway between your heart's upper chambers and lower chambers causes a rapid heartbeat. In Wolff-Parkinson-White (WPW) syndrome, an extra electrical pathway between your heart's upper and lower chambers causes a rapid heartbeat.Is avnrt hereditary?
A familial clustering of AVNRT has been reported in several families, suggesting a hereditary contribution to the development of AVNRT in some patients. In an earlier report, variable familial clusterings were observed in six families.What is a reentrant rhythm?
Atrioventricular nodal reentry tachycardia (AVNRT) is the most common type of supraventricular tachycardia. Episodes often start and end suddenly, and occur because of a reentrant circuit — also called an accessory pathway — located in or near the AV node that causes the heart to beat prematurely.What is AV nodal reentrant tachycardia?
AV-nodal reentrant tachycardia (AVNRT) is a type of abnormal fast heart rhythm. It is a type of supraventricular tachycardia (SVT), meaning that it originates from a location within the heart above the bundle of His. AV nodal reentrant tachycardia is the most common regular supraventricular tachycardia.What is sinus rhythm with short PR interval mean?
A short PR interval (of less than 120ms) may be associated with a Pre-excitation syndromes such as Wolff–Parkinson–White syndrome or Lown–Ganong–Levine syndrome, and also junctional arrhythmia like atrioventricular reentrant tachycardia or junctional rhythm.What is the bundle of Kent?
The bundle of Kent is an abnormal extra or accessory conduction pathway between the atria and ventricles that is present in a small percentage (between 0.1 and 0.3%) of the general population.Is atrial fibrillation a type of SVT?
There are three major types of SVT including: Atrial fibrillation. Paroxysmal supraventricular tachycardia (PSVT) Atrial Flutter & Atrial Tachycardia.What is the difference between sinus tach and SVT?
SVT is always more symptomatic than sinus tach. Sinus tachycardia has a rate of 100 to 150 beats per minute and SVT has a rate of 151 to 250 beats per minute. With sinus tach, the P waves and T waves are separate. With SVT, they are together.How is atrial flutter different from sinus tachycardia?
Remember- Suspect atrial flutter with 2:1 block whenever there is a regular narrow-complex tachycardia at 150 bpm — particularly when the rate is extremely consistent.
- In contrast, the rate in sinus tachycardia typically varies slightly from beat to beat, while in AVNRT/AVRT the rate is usually faster (170-250 bpm).
What is a retrograde P wave?
Junctional rhythm can be diagnosed by looking at an ECG: it usually presents without a P wave or with an inverted P wave. Retrograde P waves refers to the depolarization from the AV node back towards the SA node.What is AVRT in cardiology?
Atrioventricular reciprocating tachycardia (AVRT) is a macroreentrant tachycardia that needs an accessory pathway to bypass the regular conduction system.What does a retrograde P wave look like?
ECG Features of AJRRetrograde P waves are usually inverted in the inferior leads (II, III, aVF), upright in aVR + V1. AV dissociation may be present with the ventricular rate usually greater than the atrial rate.
How do you trigger SVT?
SVT is usually triggered by extra heartbeats (ectopic beats), which occur in all of us but may also be triggered by:- some medications, including asthma medications, herbal supplements and cold remedies.
- drinking large amounts of caffeine or alcohol.
- stress or emotional upset.
- a change in posture.
- smoking lots of cigarettes.
What is unstable SVT?
According to the American Heart Association, a patient is unstable when he presents with v-tach and a pulse, and v-tach is the cause of one or more of the following: Altered mental status. Loss of consciousness. Shock. Hypotension with symptoms of hemodyamic instability.Is avnrt life threatening?
The condition is usually not life-threatening because the fast heart rhythm is steady rather than chaotic. Effective treatments are available to manage, prevent, and sometimes cure AVNRT.How is Wolff Parkinson White Syndrome diagnosed?
WPW is usually diagnosed with a standard electrocardiogram (ECG), but specialized testing is required in some patients. The electrocardiogram — The WPW pattern can be detected by an ECG, even while the patient is in a normal rhythm. Conduction through the accessory pathway produces a characteristic ECG pattern.Is WPW a sinus rhythm?
Sinus Rhythm – Type A PatternDominant R wave in V1 — this pattern is known as “Type A” WPW and is associated with a left-sided accessory pathway.
Is Wolff Parkinson White Syndrome considered heart disease?
Wolff-Parkinson-White syndrome is a type of heart condition that you are born with. It causes rapid heart rate. Medicine can help control symptoms. Cardiac ablation can almost cure the disease in many cases.What does an SVT attack feel like?
Most people with SVT notice a rapid pulsation from the heart beating quickly in the chest. Other symptoms may include: dizziness, fainting, chest tightness or chest pain, difficulty breathing and tiredness. Some patients feel the need to pass water during an attack of SVT or soon afterwards.Can SVT cause stroke?
The most common SVTs are atrial fibrillation — a rapid, chaotic rhythm that increases the chance of having a stroke—and atrial flutter, a fast but usually regular heartbeat.Which is worse AFIB or SVT?
Atrial fibrillation can be more serious because, for some patients, it can lead to blood clots and increase stroke risk. The other types of SVT, those that occur in people with normal hearts, commonly develop in childhood or young adulthood.What is the initial drug of choice for SVT treatment?
In most patients, the drug of choice for acute therapy is either adenosine or verapamil. The use of intravenous adenosine or the calcium channel blocker verapamil are considered safe and effective therapies for controlling SVTs.What foods to avoid if you have SVT?
What are the foods you need to avoid when you have supraventricular tachycardia?- Alcohol.
- Caffeine in coffee, chocolate, and some sodas and teas.
- Spicy foods.
- Very cold drinks.
What is the best treatment for supraventricular tachycardia?
Treatment- Carotid sinus massage. Your doctor may try this type of massage that involves applying gentle pressure on the neck — where the carotid artery splits into two branches — to release certain chemicals that slow the heart rate.
- Vagal maneuvers.
- Cardioversion.
- Medications.
- Catheter ablation.